GLP-1 Receptor Agonists for Weight Loss: Top Choices and Results
GLP-1 (Glucagon-Like Peptide-1) medications have quickly gained attention as one of the most effective medical approaches for weight management. Initially developed to support people with diabetes, these treatments are now widely used to help regulate appetite, support metabolic function, and promote meaningful, long-term weight loss.
With the growing popularity of GLP-1 injections and prescription weight-loss therapies, many individuals are asking the same important question: which GLP-1 option delivers the best results?
To answer that, our medical research team reviewed the most widely used GLP-1 medications currently available. We examined clinical trial data, patient experiences, treatment costs, safety information, and real-world effectiveness. After a detailed comparison, we identified the top three GLP-1 medications for weight loss in 2026, with one option clearly standing out as the leading overall choice.

How Our Experts Tested & Ranked These GLP-1 Weight Loss Programs
To identify the top GLP-1 weight loss providers for 2026, our research team carried out a detailed comparison of the leading programs currently available. Each provider was evaluated based on key factors such as medical credibility, transparency in treatment plans, pricing clarity, quality of patient support, medication sourcing, delivery reliability, and overall customer satisfaction.
As part of our review, we examined publicly available clinical research on widely used GLP-1 medications like Wegovy and Zepbound. We also analyzed hundreds of verified user reviews from trusted platforms, reviewed subscription models for hidden costs or billing issues, and confirmed whether providers operate under the supervision of licensed medical professionals.
In addition, we assessed practical aspects such as how quickly patients can begin treatment, the availability of insurance assistance, prescription refill reliability, and the overall flexibility of each program. This ensured our recommendations reflect real-world usability rather than marketing promises alone.
After carefully weighing safety, effectiveness, affordability, and service quality, we identified the provider that offers the most balanced combination of professional medical oversight, transparent pricing, strong patient satisfaction, and access to proven GLP-1 therapies as our top choice for most users in 2026.
Test Winner 2026: Glp-1 Weight Loss Compared🏆
Features
- Finish a fast 2-minute online eligibility assessment
- Access clinically supported GLP-1 medications, including semaglutide and tirzepatide
- Have your information reviewed by a licensed clinician within 24 hours
- Receive a personalized, medically supervised weight management plan
- No waitlists, no surprise costs—full pricing transparency
- Complete the entire process online, from signup to treatment
Pros
- Simple and streamlined onboarding process
- Medical evaluation conducted by licensed clinicians
- Access to widely used GLP-1 weight loss medications
- No lengthy wait times or in-office appointments
- Upfront, transparent pricing with available cost savings
- Customized programs tailored to individual goals and needs
Cons
- Delivery timelines may vary, with occasional shipping delays during periods of high demand.
Features
- Medically supervised GLP-1 weight management
- Care provided by U.S.-based, board-certified clinicians
- Customized treatment plans tailored to individual needs
- Quick and complimentary prescription delivery
- Convenient, fully online medical consultations
- Authorized, secure, and trusted healthcare platform
Pros
- Direct access to experienced, board-certified clinicians
- No insurance needed and no complicated paperwork
- Customized care plans with continuous medical oversight
- Easy and convenient fully online process
- Clear, upfront pricing with available cost savings
- Strong patient trust backed by high satisfaction ratings
Cons
- The online care model may not be ideal for all users
- Eligibility for GLP-1 treatment can vary by individual
- Participation is dependent on clinical evaluation
- Results may differ based on personal response
- Following medical guidance is essential for best outcomes
- Should be combined with healthy lifestyle habits
Features
- Affordable access to compounded GLP-1 treatment options
- Convenient, fully online medical consultations
- Treatment supervised by licensed healthcare professionals
- Continual support with progress tracking
- Private, secure, and confidential care experience
- No clinic visits or in-person appointments needed
Pros
- Clinician-guided medical weight loss program
- Access to widely recognized GLP-1 brand-name medications
- Simple and convenient online medical consultations
- Confidential and discreet treatment process
- Suitable for individuals who haven’t achieved results with traditional dieting
- Structured program designed to support long-term consistency
Cons
- Eligibility is based on a clinical medical review
- Medication access may vary depending on location & qualification
- Results differ based on individual response & treatment
- Ongoing commitment is recommended to achieve optimal results
- GLP-1 medications may involve potential side effects
- Customer support response times can vary during peak periods
What Is GLP-1: Understanding The Biological Miracle Molecule
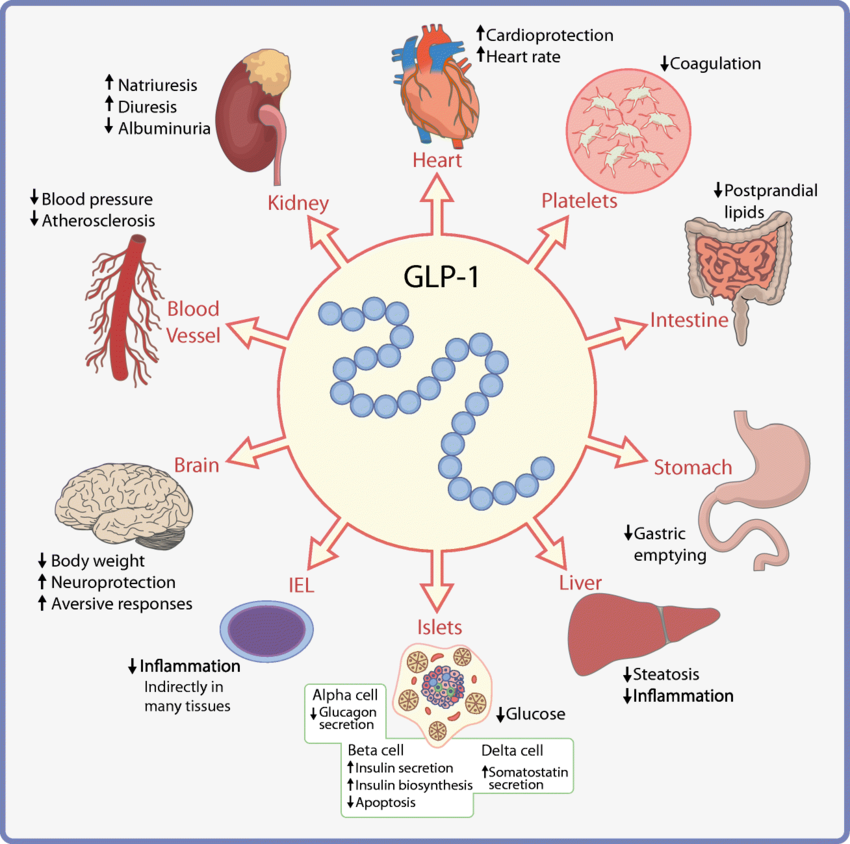
GLP-1 (Glucagon-Like Peptide-1) is an incretin hormone naturally produced by L-cells in the distal ileum and colon in response to nutrient ingestion. This remarkable molecule performs several crucial physiological functions: it stimulates glucose-dependent insulin secretion from pancreatic beta cells, inhibits glucagon secretion from pancreatic alpha cells, slows gastric emptying (thereby regulating the rate of nutrient absorption), and promotes satiety through direct action on hypothalamic centers in the brain. Essentially, what is GLP-1 medication if not a pharmaceutical replication and enhancement of this elegant natural biological process?
The fundamental breakthrough came when pharmaceutical researchers developed medications that could mimic GLP-1’s effects but with crucial pharmacological advantages: these synthetic analogs resist degradation by the DPP-4 enzyme (which normally breaks down natural GLP-1 within minutes), providing sustained therapeutic action lasting from 24 hours to an entire week depending on the specific formulation. This extended activity creates a continuous regulatory effect on appetite and blood glucose control that natural GLP-1 cannot achieve.
The Dual Mechanism of Action: How GLP-1 Medications Create Transformative Results
GLP 1 medications for weight loss operate through two primary interconnected mechanisms that create a powerful synergy for sustainable weight management. First, they significantly slow gastric emptying—the physiological process by which food transitions from the stomach to the small intestine. This delayed transit means nutrients remain in the stomach longer, creating prolonged feelings of fullness and satiety after meals, which naturally reduces overall caloric intake without conscious restriction. Second, these medications cross the blood-brain barrier and act directly on appetite regulation centers in the hypothalamus and brainstem, effectively reducing hunger signals, diminishing food cravings (particularly for high-calorie, high-carbohydrate foods), and altering reward responses to eating.
This sophisticated combination of peripheral and central nervous system effects makes GLP-1 weight loss uniquely effective and sustainable. Unlike stimulant-based weight loss pharmaceuticals that can cause tachycardia, hypertension, jitteriness, and dependency concerns, GLP-1 receptor agonists work harmoniously with your body’s intrinsic regulatory systems, resulting in fewer adverse effects and more physiologically appropriate outcomes. Additionally, research indicates these medications may increase energy expenditure slightly and promote preferential fat loss while preserving lean muscle mass—a critical distinction from many traditional weight loss approaches.
Appetite Regulation
Direct action on brain hunger centers reduces cravings and promotes natural portion control without constant willpower exertion.
Metabolic Enhancement
Improves insulin sensitivity, glucose metabolism & may enhance lipid profiles for comprehensive metabolic health benefits.
Sustainable Results
Clinical trials show maintained weight loss at 2-year follow-ups, unlike the regain common with traditional approaches.
GLP-1 Injections and Medications: A Comprehensive Clinical Guide

When patients and clinicians discuss GLP1 injections, they’re typically referring to pharmaceutical agents like semaglutide (available as Ozempic® for diabetes and Wegovy® for obesity) and liraglutide (marketed as Victoza® for diabetes and Saxenda® for weight management). These medications are administered via subcutaneous injection using proprietary injection pens with ultra-fine needles that most users describe as causing minimal discomfort—comparable to or less than routine fingerstick glucose testing. The convenience of once-weekly dosing (for semaglutide) has revolutionized adherence rates compared to daily injection regimens, making these medications particularly suitable for individuals with demanding schedules or needle apprehension.
Understanding the Expanding Landscape of GLP-1 Medications
The therapeutic landscape of GLP 1 medications has expanded dramatically since the first agent (exenatide) received FDA approval in 2005. While all GLP-1 receptor agonists share the same fundamental mechanism of action—mimicking endogenous GLP-1 hormone activity—different medications exhibit varying pharmacokinetic profiles, durations of action, administration frequencies, and specific regulatory approvals. Some agents like semaglutide and dulaglutide are approved specifically for weight management in individuals with or without type 2 diabetes, while others like lixisenatide are primarily indicated for glycemic control with weight-neutral effects. The newest generation of dual- and triple-agonist medications demonstrate even more pronounced weight loss effects in clinical trials, potentially representing the next evolution in this therapeutic class.
What is the best GLP 1 for weight loss? A Clinical Perspective
Determining the best GLP 1 for weight loss requires careful consideration of numerous individual factors including medical history, concomitant conditions, weight loss objectives, lifestyle considerations, insurance coverage, and personal tolerance profiles. Clinical trials have demonstrated varying efficacy among different agents, with higher-dose semaglutide (2.4mg weekly as Wegovy®) showing superior weight loss outcomes compared to liraglutide (3.0mg daily as Saxenda®) in head-to-head studies. However, the optimal medication is ultimately the one that produces effective results for an individual with acceptable side effects and sustainable access. Clinical guidelines increasingly recommend shared decision-making between patients and providers when selecting among available options.
GLP 1 pros and cons: A Balanced Clinical Assessment
A comprehensive understanding of GLP 1 pros and cons is essential for informed treatment decisions. The substantial advantages include clinically significant weight loss (typically 10-15% of baseline body weight), improved glycemic control (with potential reduction or elimination of diabetes medications), reduced cardiovascular event risk (demonstrated in outcomes trials), decreased appetite and food preoccupation, and potential metabolic benefits extending beyond weight management. Potential considerations include gastrointestinal side effects (particularly nausea during dose escalation, though usually transient), cost and insurance coverage challenges, the requirement for ongoing treatment to maintain benefits (similar to hypertension or lipid medications), and the need for proper injection technique and storage.
Common Side Effects
Nausea (usually transient), constipation, diarrhea, and occasional injection site reactions that typically diminish over time.
Rare Considerations
Gallbladder issues, pancreatitis risk (extremely rare), and potential thyroid C-cell tumor concerns.
Evolving GLP-1 Therapeutic Landscape

When examining semaglutide brand name pharmaceuticals, we encounter Ozempic® (approved for type 2 diabetes management) and Wegovy® (FDA-approved specifically for chronic weight management in adults with obesity or overweight with at least one weight-related condition). These medications contain the same active ingredient (semaglutide) but differ in their indicated dosing regimens and approved uses. Ozempic® is typically prescribed at doses up to 1mg weekly for glycemic control, while Wegovy® utilizes a specific titration schedule up to 2.4mg weekly for weight management. The STEP clinical trial program (Semaglutide Treatment Effect in People with obesity) demonstrated unprecedented weight loss results, with participants losing an average of 14.9% of body weight at 68 weeks—nearly double the efficacy of previously available pharmacotherapies.
Which GLP-1 is Approved for Weight Loss? Regulatory Landscape
Patients frequently inquire which GLP 1 is approved for weight loss specifically. The current FDA-approved landscape for weight management includes liraglutide (Saxenda®, approved 2014), semaglutide (Wegovy®, approved 2021), and, more recently, tirzepatide (Mounjaro®, with weight management approval under review after demonstrating up to 22.5% weight loss in SURMOUNT trials). Additionally, several GLP-1 receptor agonists including dulaglutide (Trulicity®) and exenatide extended-release (Bydureon®) are approved for type 2 diabetes with weight loss as a beneficial secondary effect. The regulatory environment continues to evolve rapidly as new agents and formulations complete clinical development, promising even more options in the coming years.
Which GLP 1 is best for weight loss? Evidence-Based Analysis
The question of which GLP 1 is best for weight loss lacks a universal answer but benefits from evidence-based analysis. Direct comparison trials like STEP 8 demonstrated that semaglutide 2.4mg weekly produced significantly greater weight reduction than liraglutide 3.0mg daily (15.8% vs. 6.4% at 68 weeks). However, individual variability in response, side effect profiles, dosing preferences (daily vs. weekly), cost considerations, and insurance coverage substantially influence the optimal choice. Emerging data suggests that dual-agonist medications like tirzepatide may offer superior efficacy, though longer-term data and broader real-world experience are still accumulating. The principle of personalized medicine applies strongly here—the best medication aligns with an individual’s specific physiology, lifestyle, and treatment goals.
The Complete GLP-1 Journey: A Realistic Week-by-Week Expectation Guide
Initiating GLP-1 therapy represents a journey that unfolds over weeks and months, with distinct phases characterized by physiological adaptation, dose optimization, and eventual maintenance. Understanding this progression helps establish realistic expectations, prepares individuals for common experiences, and promotes long-term adherence—critical factors for achieving optimal outcomes.

Weeks 1-4: The Physiological Adaptation Phase
During the initial month, your body undergoes gradual adaptation to the medication’s effects. Most protocols begin with a conservative starter dose specifically to minimize gastrointestinal side effects as your system adjusts. Common experiences during this period include mild appetite reduction, early modest weight loss and possible transient nausea or digestive changes that usually diminish within days to weeks. Many individuals report the most noticeable initial effect as reduced “food noise”—the constant mental preoccupation with eating that often accompanies weight struggles. Hydration becomes particularly important during this phase, and many clinicians recommend splitting meals into smaller, more frequent portions to accommodate slowed gastric emptying.
Weeks 5-12: Dose Escalation and Building Momentum
Following the initial adaptation period, most protocols involve gradual dose titration toward the target maintenance dose. As medication levels increase physiologically, therapeutic effects become more pronounced and consistent. Weight loss typically accelerates during this period, with many individuals losing 1-2 pounds per week—a rate considered optimal for sustainable results and minimizing lean muscle loss. Energy levels often improve noticeably as metabolic parameters shift, and clothing may begin fitting differently, providing positive reinforcement. This phase often involves establishing new eating patterns that align with natural appetite signals rather than external diet rules. Many individuals discover they naturally prefer smaller portions, experience diminished cravings and find healthy choices more appealing.
Months 3-6: Therapeutic Optimization and Significant Transformation
By month three, most individuals have reached their maintenance dose and experience the medication’s full therapeutic effects. Weight loss continues at a steady, sustainable pace, with clinical trial data showing average losses of 5-10% of initial body weight by month six—a threshold associated with clinically significant health improvements. Beyond scale weight, health metrics typically show marked improvement: blood pressure reductions of 5-10 mmHg, LDL cholesterol decreases of 10-20%, hemoglobin A1C reductions of 1.0-1.5% in those with diabetes or prediabetes, and decreased inflammatory markers. Many report improved mobility, reduced joint pain, better sleep quality, and enhanced mood—benefits extending far beyond weight measurement alone. This period often involves refining lifestyle habits that support long-term maintenance.
Month 6 and Beyond: Maintenance, Lifestyle Integration, and Long-Term Strategy
Beyond six months, weight loss typically continues at a gradual pace before eventually plateauing at a new physiological set point. The focus strategically shifts toward maintaining achieved results and seamlessly integrating sustainable habits into lifelong patterns. Many individuals continue medication at the maintenance dose to sustain benefits, as GLP-1 receptor agonists work ongoingly rather than providing a permanent metabolic “reset.” This period emphasizes behavioral sustainability: establishing consistent physical activity routines, developing mindful eating practices that honor natural hunger/fullness cues, managing stress through non-food mechanisms, and cultivating a supportive environment. Regular follow-up with healthcare providers ensures optimal dosing, monitors for potential side effects, and addresses any emerging questions or challenges.
It’s essential to recognize that individual experiences vary based on numerous factors including baseline characteristics, genetic predispositions, adherence to medication and lifestyle recommendations, and individual metabolic responses. Some individuals respond more dramatically than clinical averages, while others experience more modest effects. The journey isn’t linear—weight plateaus and occasional fluctuations are normal and expected. What distinguishes GLP-1 therapy from previous approaches is the physiological foundation that makes sustained adherence and long-term success more achievable for most individuals.
Advanced GLP-1 Strategies: Microdosing, Accessibility, and Future Directions
Microdosing GLP-1: A Personalized, Gentle Initiation Strategy
The concept of microdosing glp 1 has gained attention among individuals particularly sensitive to medication effects or those wishing to minimize initial side effects. This approach involves initiating therapy at doses lower than the manufacturer’s recommended starting dose, then titrating upward more gradually than standard protocols. While not an officially approved administration method, some experienced clinicians employ this strategy for patients who experience pronounced gastrointestinal side effects at standard starting doses or those with heightened sensitivity to medications generally. Microdosing may involve using insulin syringes to administer partial doses from prefilled pens or utilizing compounded formulations at customized concentrations. It’s crucial that any dose modification occurs under medical supervision, as improper dosing can compromise efficacy or safety.
Best GLP-1 for weight loss over the counter: Understanding Limitations
Many individuals search for the best glp 1 for weight loss over the counter, highlighting the significant demand for accessible weight management solutions. However, it’s medically important to clarify that authentic, pharmaceutical-grade GLP-1 receptor agonists are prescription-only medications with rigorous FDA oversight regarding manufacturing, purity, dosing accuracy, and clinical evidence. Various dietary supplements and “research chemicals” marketed online may claim to contain GLP-1 analogs or boost endogenous GLP-1 production, but these products operate in a regulatory gray area without proven safety or efficacy standards. Their chemical composition, purity, concentration accuracy, and biological activity remain uncertain and potentially risky. Individuals considering such options should consult healthcare professionals about legitimate pathways to access evidence-based treatments, including patient assistance programs, insurance advocacy, or clinical trials for those facing financial or coverage barriers.

GLP-1 vs. Traditional Weight Loss Approaches: Paradigm Shift
Comparing GLP-1 pharmacology to traditional weight management approaches reveals a fundamental paradigm shift in both mechanism and outcomes. Conventional diet and exercise strategies primarily address energy balance through behavioral modification and conscious caloric restriction—approaches that often trigger powerful biological counter-regulatory responses (increased hunger, reduced metabolic rate) that undermine long-term success for many individuals. In contrast, GLP-1 medications work at a physiological level to reduce appetite and enhance satiety signals, thereby making sustainable caloric reduction more achievable by aligning with rather than fighting biological drives. This doesn’t negate the importance of nutrition and activity—rather, it creates a physiological environment where adopting healthier behaviors becomes more natural and sustainable. The integration of medication with lifestyle intervention typically yields superior outcomes to either approach alone, representing a modern comprehensive model for obesity management.
Future Directions: The Expanding Horizon of GLP-1 Therapeutics
The rapid evolution of GLP-1-based therapeutics continues with several promising developments on the horizon. Oral formulations of semaglutide (Rybelsus®) already exist for diabetes and may expand to weight management. Next-generation agents combining GLP-1 activity with other incretin pathways (GIP, glucagon) show enhanced efficacy in clinical trials. Research explores potential applications beyond obesity and diabetes, including neurodegenerative conditions (Alzheimer’s, Parkinson’s), addiction disorders, non-alcoholic steatohepatitis (NASH), and cardiovascular protection independent of weight effects. Additionally, sustained-release formulations requiring less frequent administration (monthly or longer) are in development. The growing recognition of obesity as a chronic disease requiring long-term management parallels the maturation of these therapeutic options, promising increasingly personalized and effective approaches in coming years.
GLP-1 Frequently Asked Questions: Evidence-Based Answers
How quickly will I see results with GLP-1 medications?
Most individuals notice initial appetite reduction within the first 1-2 weeks, with measurable weight loss typically beginning within the first month. Clinical trial data shows average weight loss of approximately 5% of body weight by 3 months and 10-15% by 6-12 months with appropriate dosing and lifestyle integration. Individual responses vary based on factors including specific medication, dose, adherence, baseline characteristics, and concomitant lifestyle modifications.
Are GLP-1 medications safe for long-term use?
Current evidence from clinical trials extending to 2+ years demonstrates favorable safety profiles for approved GLP-1 receptor agonists when used as directed under medical supervision. Like all medications, they carry potential side effects (primarily gastrointestinal) that typically diminish over time. Certain individuals with specific medical histories (personal/family history of medullary thyroid cancer or Multiple Endocrine Neoplasia syndrome type 2) should avoid these medications. Ongoing surveillance studies continue to monitor long-term outcomes, but current data supports their use as chronic therapies for chronic conditions.
What happens if I stop taking GLP-1 medications?
Discontinuation typically leads to gradual return of appetite and eventual weight regain, as these medications provide ongoing physiological effects rather than permanent metabolic alteration. This pattern parallels other chronic disease medications—stopping blood pressure medication leads to blood pressure returning to previous levels. For this reason, obesity medicine specialists generally recommend continued treatment to maintain benefits, though dose adjustments may occur during maintenance phases. Some individuals may successfully maintain results after discontinuation with intensive lifestyle support, but this varies considerably.
Can GLP-1 medications be used with other weight loss approaches?
GLP-1 receptor agonists are frequently combined with comprehensive lifestyle interventions (nutrition counseling, physical activity, behavioral strategies) for synergistic effects. They may also be combined with other weight management medications in certain clinical scenarios under specialist supervision. However, combination with other appetite suppressants requires careful medical oversight due to potential additive effects. These medications are generally not combined with surgical weight loss procedures in the immediate postoperative period but may be used later for weight regain management.
Final Consideration:
Before starting any GLP-1 therapy, it’s essential to consult with a licensed healthcare professional. They can evaluate your health background, explain the potential advantages and possible risks, and help determine whether this treatment is the right fit for your individual needs.
Our program is designed to assist throughout this process by providing clear educational materials, access to qualified clinicians, and continuous support—helping you use GLP-1 medications safely while working toward effective, long-term weight management.
Experts Recommendation
RemedyMeds
Features
- Finish a fast 2-minute online eligibility assessment
- Access clinically supported GLP-1 medications, including semaglutide and tirzepatide
- Have your information reviewed by a licensed clinician within 24 hours
- Receive a personalized, medically supervised weight management plan
This website may earn compensation from certain offers and links displayed. Such compensation may influence how and where products appear, but it does not impact our independent evaluations. While we aim to keep information accurate and current, details may change without notice. Always review the provider’s terms and conditions before proceeding.
Disclaimer | Terms & Conditions | Contact Us | Privacy Policy
Copyright © 2026


